People with diabetes are more susceptible to heart disease. But through medical intervention and lifestyle changes, diabetics can learn to take better care of their heart.

Adults with diabetes are two to four times more likely to die from heart disease than those without. While diabetics are more likely to develop heart disease, those with type 2 diabetes are particularly at risk.
Coronary artery disease (CAD) is, in fact, the cause of death in more than half the patients with diabetes. In one study, it was shown that at least 68% of people aged 65 and older with diabetes die from some sort of heart disease and 16% die of stroke.
Studies also show that the risk of heart attack in diabetics is equivalent to that of non-diabetics with a prior history of heart attack. Women with diabetes also have an increased risk, with one study indicating that they have a risk of cardiovascular death of up to 7.5 times more than women without diabetes. It appears that women with diabetes do not possess the pre-menopausal benefit seen in the general female population.
HOW DOES DIABETES LEAD TO HEART DISEASE?
Diabetes is treatable, but even with glucose levels under control, the risk of heart disease is present. This is because diabetes causes wear and tear of blood vessels, which translates to the heart having to work a lot harder.
In Asia, type 2 diabetes usually occurs in the setting of metabolic syndrome, which is a cluster of conditions — hypertension, high blood sugar, excess body fat around the waist, and abnormal cholesterol levels — that occur together, raising one’s risk of developing diabetes, which in turn increases the likelihood of heart disease. This is also known as insulin resistance syndrome, or Syndrome X.
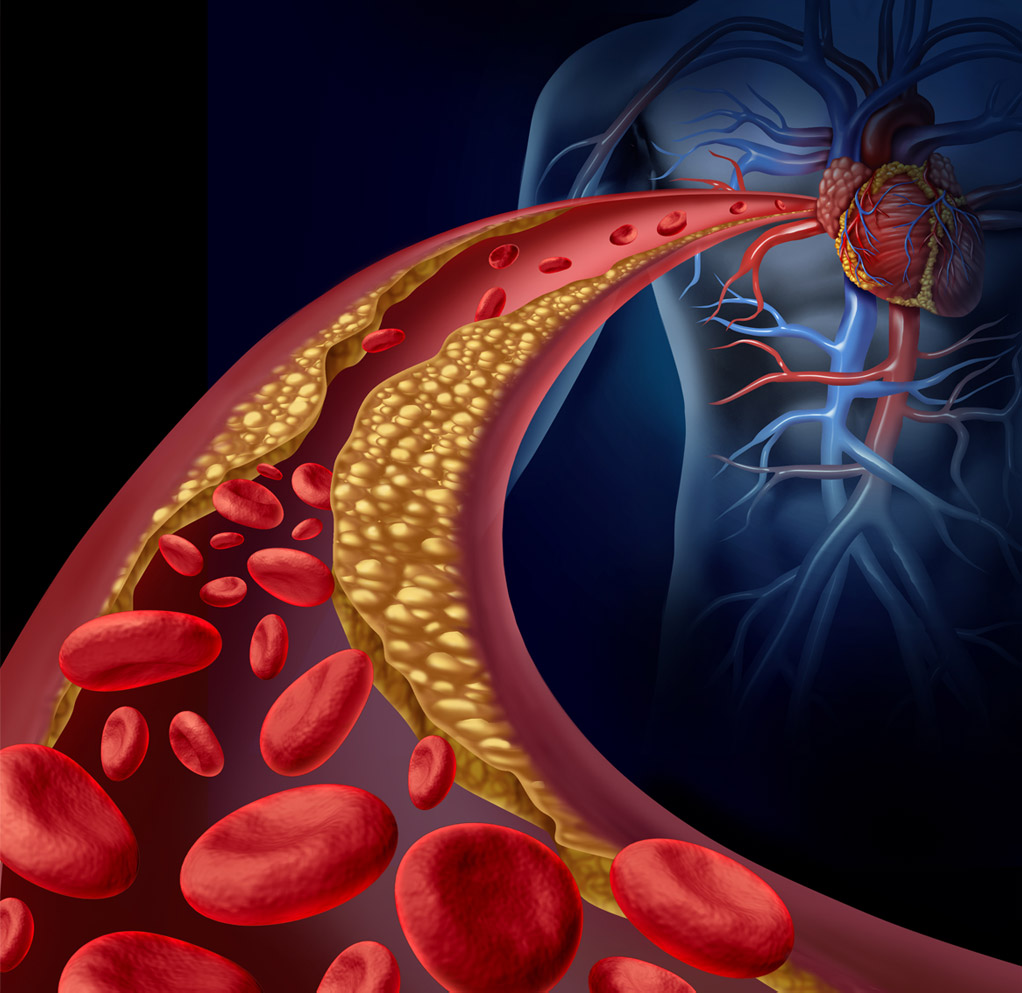
The most common cause of heart disease in a diabetic is hardening of the coronary arteries, or atherosclerosis. This is caused by a build up of plaque (fat, cholesterol, calcium and other substances) in the blood vessels, which supply oxygen and nutrition to the heart.
When the plaque breaks apart, the body tries to repair the rupture by sending platelets to seal it up. As the artery is small, the platelet plug could block the flow of blood, hence preventing oxygen delivery, and a heart attack happens.
Symptoms of a heart attack include shortness of breath, feeling faint, nausea, excessive and unexplained sweating, and pain in the chest, shoulders, jaw and left arm.
Diabetes, on the other hand, may not cause the typical symptom of chest pain, and this is described as silent ischaemia or silent heart attack. This results in a late presentation, which contributes to a higher mortality (risk of dying). Several studies of silent ischaemia have shown that CAD severity, and myocardial infarction (heart attack) and death rates are the same in patients with silent ischaemia and those with symptomatic ischaemia.
Diabetes-related nerve damage that blunts the heart pain may explain why symptoms are not noticed. People with diabetes may also have reduced myocardial blood flow, a reflection of suboptimal coronary vasodilatory capacity.
Diabetics who present with heart attacks are at an increased risk of dying from their cardiac event or developing heart failure, a serious condition where the heart cannot pump blood adequately. This can lead to fluid build up in the lungs, which causes difficulty in breathing, fluid retention, and swelling in other parts of the body (especially the legs). Patients with diabetes also have a higher incidence of multi-vessel disease and greater number of diseased vessels.
Early screening and detection of CAD in diabetics is important to ensure that appropriate medical treatments and interventions to improve outcome are carried out. This is particularly so for diabetics who participate in high-intensity sports.
10 WAYS TO PREVENT PROBLEMS
The best measure to avoid diabetes-led heart disease is to manage the condition and look after your health. Here are some ways to do so:
- Keep your blood sugar at a healthy level
Monitor your blood sugar level daily to assess how it is affected by foods and activities, and if the treatment plan is working. - Get your blood pressure and cholesterol levels under control
Medications, if necessary, must be taken. - Maintain a healthy weight and lose some pounds if necessary
Obesity is a major risk factor for cardiovascular disease and has been associated with insulin resistance. If you are overweight, shedding a few kilos can boost your body’s ability to use insulin, lower blood sugar level, and improve blood pressure and lipids levels. - Seek a doctor’s advice to reduce risk of heart disease
Check if you need medications, such as aspirin, to protect against cardiovascular conditions. - Exercise regularly
This helps to better control blood sugar level and reduce the risk of cardiovascular disease. Muscles that are working use more glucose than those that are resting, thus the greater sugar uptake by muscle cells lowers blood sugar levels. Exercise is also beneficial for weight control and stress management. You should complete 150 minutes of moderate-intensity aerobic activity (exercising at a level that raises your heart rate and makes you perspire) every week. This includes light jogging, brisk walking, cycling, and water aerobics. - Adopt a heart-healthy diet
Control portion size, eat more fruits and vegetables, choose wholegrain products, limit intake of saturated and trans fats, select low-fat protein sources, and reduce sodium intake. Drink alcohol in moderation. Allow yourself an occasional treat and you will find that heart-healthy eating is both possible and enjoyable. - Quit smoking
Smoking puts you ― whether or not you have diabetes ― at higher risk of heart disease and stroke. Learn about smoking cessation programmes and tools. Non-smokers should stay away from second-hand smoke. - Manage and reduce stress
Stress can cause blood glucose levels in diabetics to rise. Get rid of physical or mental stresses through relaxation techniques, such as breathing exercises, yoga and meditation. - Take medications as prescribed and keep to your appointments
Update your doctor on how you are doing during each visit. - Get enough sleep
Lack of sleep can increase your craving for sugar and high-calorie foods, even when your body does not need them. This can lead to weight gain and insulin resistance.







