Eczema causes red, itchy and scaly patches of rash that can cause major discomfort.
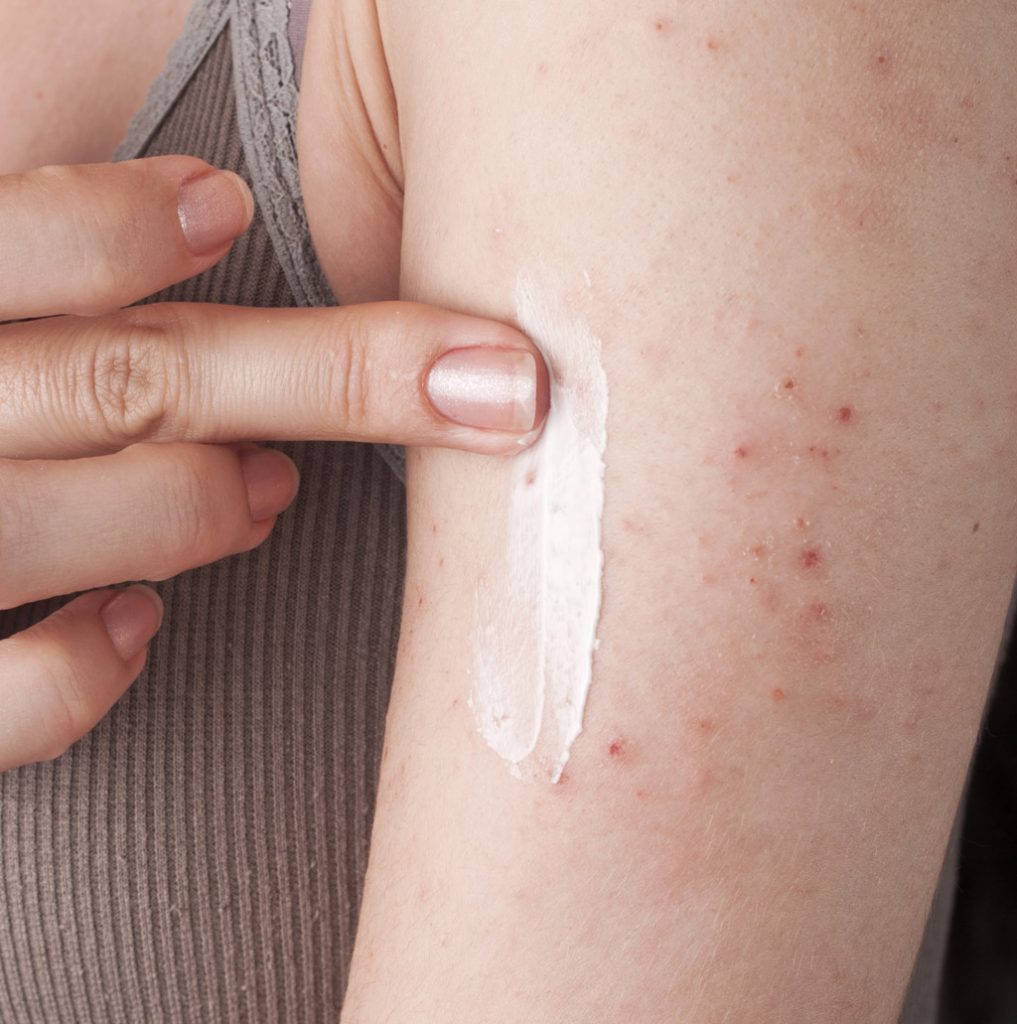
More than just a heat rash, eczema is an itchy inflammatory skin condition. The term actually refers to a broad group of skin disorders known as dermatitis – ‘derma’ for ‘skin’ and ‘-itis’ for ‘inflammation’. The rash often appears as red, bumpy and peeling patches of skin and can be severely itchy. The rash is not infectious and can be caused by a wide range of internal or external factors.
Many forms of eczema are caused by an abnormal response of the skin’s immune system and impaired skin barrier function. This can be due to genetics or to aggravating factors such as stress, skin dryness, irritating soaps, detergents or chemicals, scratchy or woolly clothing, changes in temperature or humidity, certain foods, or an overgrowth of certain bacteria or yeast.
Types of eczema
There are several types of eczema. The most common is atopic eczema. Others include discoid eczema, seborrhoeic eczema, contact dermatitis and vesicular eczema of hands and feet. These are all characterised by itchiness, redness, skin swelling, scaliness, small bumps called papules, oozing and crusting.
- Atopic eczema commonly starts in childhood and affects about 20% of school children in Singapore. The rash is severely itchy, red, dry and scaly, and the affected skin can become wet and weepy, or painful. The rash can appear on the limbs, knees and elbows, as well as on the scalp, eyelids, ears, trunk, fingers and toes. This form of eczema is chronic and recurrent and often occurs alongside other inherited hypersensitive conditions such as allergic rhinitis, allergic conjunctivitis or asthma.
- Asteatotic eczema causes cracking and resultant inflammation. It is due to skin dryness which is a natural part of ageing and typically affects older people.
- Discoid eczema tends to occur in young people and may be set off by insect bites. It causes very itchy circular red patches of little blisters or red spots that quickly become scratched and weepy, or dry and crusted.
- Exogenous eczema is caused by environmental allergens or irritants. For instance, allergic contact dermatitis is due to skin allergy to substances such as perfume or nickel.
Management and prevention
For all types of eczema, the best treatment involves a multipronged approach and in recent years, there has been a paradigm shift from reactive treatment to proactive treatment. The focus has moved to preventing the outbreak by using skin barrier-repairing moisturisers in conjunction with intermittent topical steroids or steroid-free topical immunomodulators. Such treatment methods have been shown to prolong the interval between outbreaks and reduce the frequency of outbreaks.
For eczema caused by external factors, called exogenous eczema, treatment involves first identifying the allergens or stimuli that cause the outbreak and avoiding these. The diagnosis is made through a careful and detailed history and a patch test which involves applying tiny concentrations of common allergens to the skin. The skin is then observed for a reaction. Treatment may also involve creams or medications to treat the symptoms. For endogenous eczema, where the cause is internal, there is no cure identified to date. However, an eczema episode can usually be brought into remission using topical steroids, treatment of infections and good general skincare.
Topical steroids, however, can sometimes cause skin thinning and other side effects. As such, they should only be used in the long run under an experienced doctor’s supervision. If topical steroids are insufficient, a dermatologist is recommended. Depending on the patient’s profile, alternative options such as UVB phototherapy or oral medications – ranging from oral antibiotics and short-term oral steroids to oral immunomodulatory medication – may be used.







