Myopia

Nearsightedness, or myopia, is the most common eye disorder whereby close objects can be seen clearly, while objects farther away appear blurred.
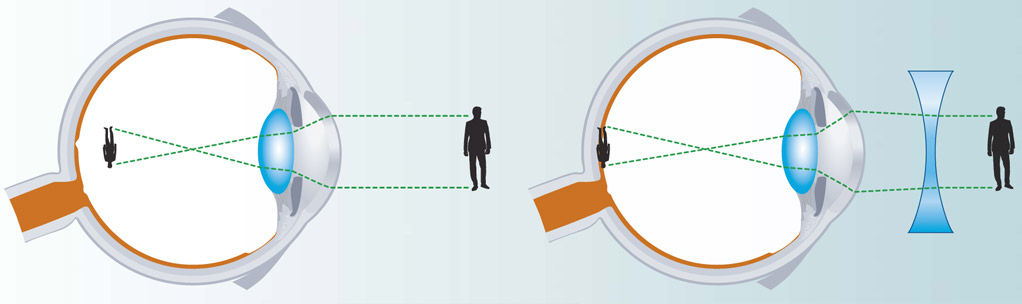
Myopia affects close to half of all Singaporean children aged nine years old — a huge number compared to Western populations, where less than 5 per cent of children have this affliction. And even though childhood myopia typically occurs from age six, there is a worrying trend that myopia is affecting even younger children.
Progressive childhood myopia is attributed to a combination of genetic and environmental factors; a child is more likely to develop myopia if he/she has one or both parents who suffer from myopia and is constantly involved in near work — activities that require his/her eyes to be focused on a spot near them.
Children born prematurely, with rare cases of inherited diseases of the retina, or genetic disorders like Down Syndrome, are also at a higher risk of having myopia, said Dr Leo.
The earlier the onset and the faster the rate of progression, the more myopic the child becomes — and the higher the risks of developing complications which lead to reduced vision and blindness. These include retinal detachment, cataracts at an earlier age, glaucoma and macular degeneration among others. In young children less than seven years old, if the difference in the degree of myopia in both eyes is big, it can lead to permanent visual loss in a condition called amblyopia or “lazy eye”.
Early diagnosis allows optical aids such as spectacles and contact lenses to be used to correct the child’s vision. More importantly, interventions to slow down the progression of myopia can be proposed, such as minimising near work and increasing outdoor play instead.
If the myopia rapidly progresses despite these measures, atropine eyedrops may be prescribed by the eye doctor. Some studies suggest that atropine eyedrops is the most effective method to slow down myopia progression, said Dr Leo. Furthermore, a recent two-year study showed that the use of atropine 0.01 per cent seemed to have no side effects at all, which makes it a promising treatment. The dose available ranges from atropine 0.01 to 1 per cent. Patients can expect an average of 50 to 60 per cent reduction in progression and in some cases, the myopia may not progress at all.
CATARACTS
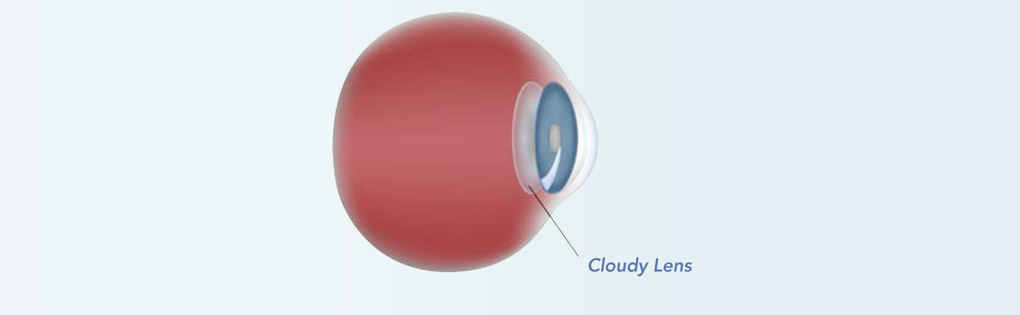
Cataracts are clouding of the natural lens of the eye and it affects more than 80 per cent of Singaporeans who are over 60 years old. Although age is the most common contributing factor to developing cataracts, diabetes, smoking, overexposure to sunlight and certain medications, such as steroids, can also cause cataracts.
In rare cases, infants and children can also have cataracts. These congenital cataracts can be due to many causes like infections, chromosomal abnormalities, or a more extensive syndrome or disease.
Cataract surgery is the single most effective method to correct the condition as it never subsides on its own. If left untreated, cataracts cause deteriorated vision, and eventually, blindness.
Traditionally, cataract surgery involves surgically removing the cloudy lens and replacing it with an artificial implant, known as intraocular lens (IOL).
More recently, there is “bladeless” surgery, which utilises femtosecond laser technology to remove cataracts. Femtosecond lasers emit optical pulses of extremely short duration (as short as one-quadrillionth of a second) and these ultra-short yet intense bursts of near-infrared light pulses allow tissue to be cut more precisely with negligible heat. This technology has already been used widely in refractive surgery (LASIK) and looks set to revolutionise cataract surgery as well. During surgery, the computer-guided femtosecond laser makes openings in the eye (cornea incisions) that can be programmed to be a precise shape. The femtosecond laser is also able to create a perfect, round opening in the front of the lens and break up the lens into pieces. The dissolved cataract is subsequently removed with phacoemulsification.
All this is done with an image guidance system (optical coherence tomography, OCT ) that provides real-time three-dimensional and high-resolution images of the eye.
However, prior to delivering the laser, a patient’s eye must be prepped by using a curved lens and suction system. Patients with cornea disease, glaucoma and who cannot tolerate or cooperate with the preparation procedures are not suited to undergo the laser surgery. Another disadvantage is the increased cost of the surgery, said Dr Leo.
She added that if there is no other reason causing the vision impairment like retinal problem or poorly controlled high eyeball pressure, vision will be effectively restored with surgery.







