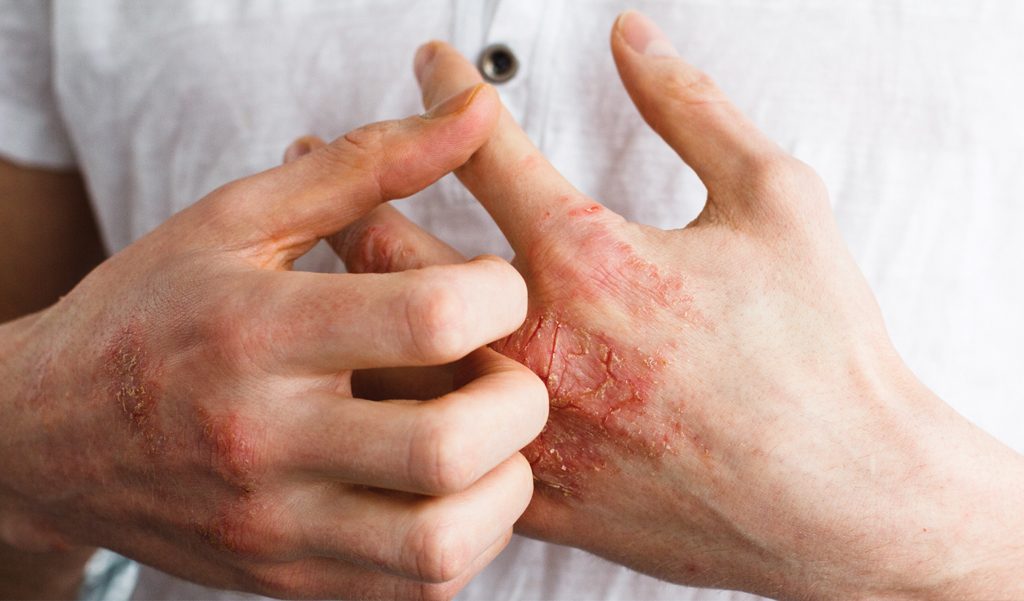
Psoriasis is an inflammatory condition where the replacement of skin cells is vastly accelerated. It is characterised by red, scaly patches of skin, and affects about 2–3% of the population. About 125 million people worldwide have the condition.
Psoriasis affects all races, genders and ages, but begins more frequently between the ages of 15 and 45, particularly during puberty and menopause; it affects children, too.
Accompanied by irritation or itch, the severity of psoriasis may vary considerably from person to person. Sometimes, if the patches are thick and dry, they crack and become sore.
Multiple causes
Psoriasis is attributed to multiple causes. While some may have inherited genes that increase their likelihood of developing psoriasis, other factors are just as significant in triggering the condition.
Aggravating factors that can cause flare-ups include stress, injury, irritation, infection, climate, hormonal changes, drugs, obesity, alcohol and smoking. Psoriasis is neither infectious nor contagious, and is not caused by poor standards of hygiene.
Other effects
Psoriasis is increasingly recognised as a chronic inflammatory disease that affects more than the skin. For example, 15–40% of sufferers may develop inflammation of the joints, or arthritis. The risk is higher in those with a family history of psoriatic arthritis or nail psoriasis. Psoriasis patients also have a greater chance of developing diabetes, high blood pressure, and heart disease.
As psoriasis tends to persist and recur, patients may be impacted economically and socially, leading to social withdrawal and feelings of seclusion, depression and embarrassment. In some cases, the psychological distress can be harder than the physical suffering.
Treatment options
Typical treatments include topical medications, phototherapy, photochemotherapy (PUVA), and oral or injectable medication (for moderate to severe psoriasis, or when joints are involved).
Biologics derived from human or animal proteins that can be self-injected are the latest and most effective treatment for moderate to severe cases of psoriasis that do not respond to conventional therapy, psoriasis associated with arthritis, or when patients display unacceptable side effects to conventional therapy. Biologics work by targeting and inhibiting overactive immune cells in the body. The newest biologics are able to achive 100% clearance in up to half of those treated, and clear/almost clear in nine out of 10 patients.
Oral or injected steroids are best avoided as they can cause unstable psoriasis and severe flare-ups upon withdrawal of the steroids.
It is best to consult a dermatologist for extensive psoriasis or psoriasis that does not respond to first-line cream treatments. Psoriasis is a chronic condition, and treatment efficacy must be balanced against long-term side effects.







